By Emily Park
Around Thanksgiving, I found myself sure that the COVID test I had just taken was going to come back positive—an assumption that came very close to ending my life at 23 years old. Because of the pandemic, I waited far too long to seek medical attention and experienced delays in my care due to the hospital being overwhelmed by the virus.
I had all of the major symptoms the CDC had been drilling into our heads for the last nine months: shortness of breath, a cough, body aches, an elevated temperature, severe exhaustion, an increased heart rate—the works. But it also turns out that all of the above are also symptoms of a pulmonary embolism (aka blood clots in the lungs), which is the third most common cause of cardiac death.
After a few days of symptoms, I had a virtual visit with my doctor who strongly predicted the COVID test she ordered would come back positive. I was only 23, had no history of clots, and COVID was rapidly spreading through the community. There wasn’t much reason to assume it was anything besides the virus.
I had both a regular and rapid test done, and a week later, both had come back negative—even though I was still experiencing all of the COVID symptoms. I scheduled another doctor’s appointment, and the nurse practitioner ordered a chest x-ray and labs that I never made it to.
Instead, I passed out in my dining room shortly after I hung up the call with the nurse. The next thing I remember is waking up on the floor with my boyfriend yelling at me to breathe. We rushed to the ER.
After going over all of this with the nurses and doctors in the ER, they were convinced the COVID tests were false negatives. They ordered another test as well as a CT, chest x-ray, and labs.
A few hours later I had an answer. I had a massive, bilateral pulmonary embolism, which meant that I had a blood clot stretching through both my right and left lungs that was working its way into the branches of all five lobes. In layman’s terms, one giant clot that was days, if not hours, away from killing me. The chest CT also revealed that the right side of my heart was enlarged due to the largest part of the clot restricting so much blood flow through the right side of my lungs.
I got this news sitting alone in a hospital bed at the end of a hallway facing an emergency exit door. Due to COVID-19, there wasn’t a room available in the ER, and I was placed where they had space—the hallway. And again, because of COVID restrictions, I wasn’t allowed to have anyone else with me.
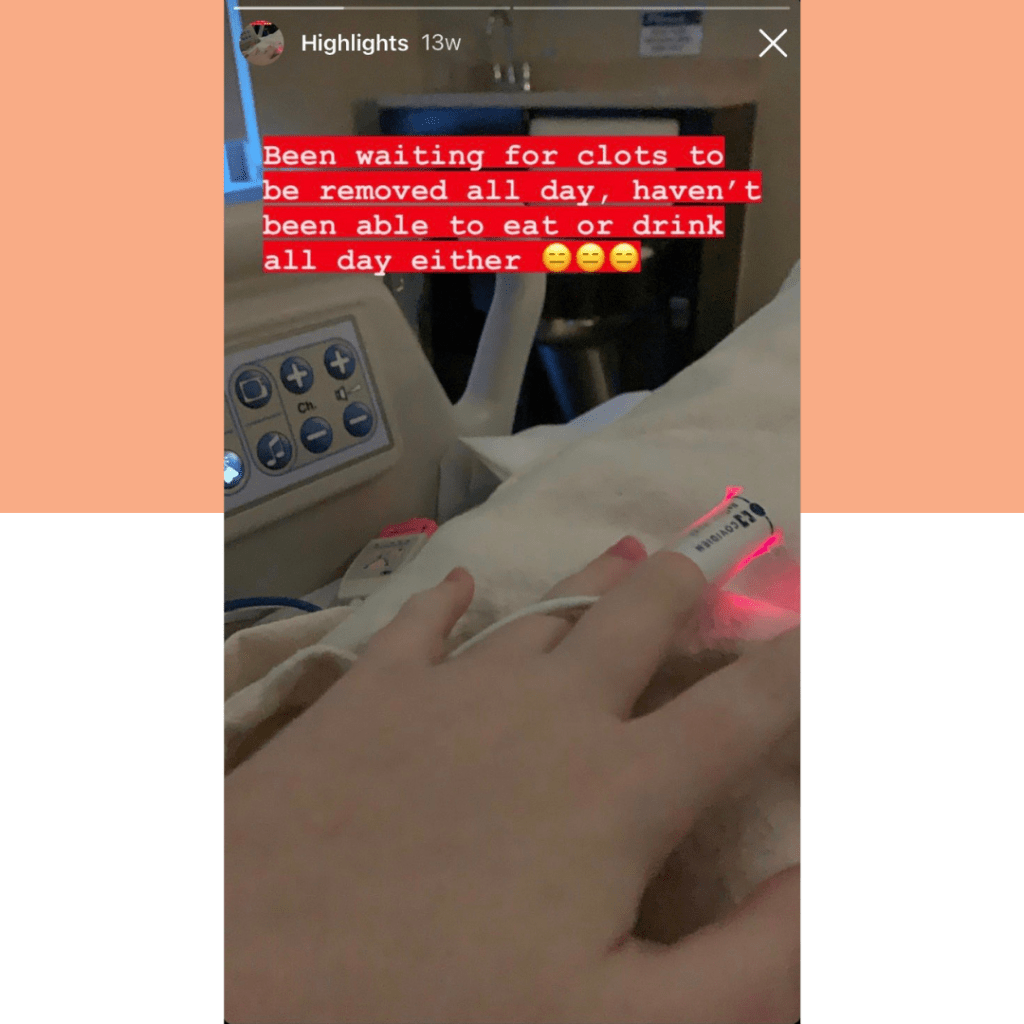
I was surprisingly calm. Honestly, I think I was in shock. A blood clot was definitely not what I was expecting. I calmly asked the nurse, “So, uh, what do we do now?” Cue nervous laughter. She told me that the blood clot was very large and very serious. There was a good chance I would have to undergo a procedure to remove the clots, and I would immediately be placed on blood thinners and likely continue taking them for the next six months, possibly the rest of my life.
I was also informed that they didn’t have room for me in their intensive care unit—which was a big “oh shit” moment for me. I’d never even stayed in a hospital, and suddenly I was getting a ticket straight to the ICU? Wild.
Since the hospital was out of beds (again due to there being so many people with COVID that had already filled their ICU), the nurse strongly suggested that I sign the papers to allow them to transfer me—by ambulance—to one of their sister hospitals about 25 minutes away. I later got a $600 bill for that ambulance ride—yay for American healthcare.
At this point, I was still waiting for the results of the COVID test, but the nurse told me it was uncommon for a patient of my age to have a blood clot that large, and there was still a good chance it was a complication of COVID.
I got the test results back when I arrived at my room at the new hospital, the COVID tests (they had taken two) had come back negative. That made four negative tests. I did not have COVID-19, I was simply “lucky” enough to have a life-threatening health emergency that mirrored the symptoms of the virus.
I was in the hospital a total of five days—two and a half in the ICU and the rest on the cardiovascular floor. While in the hospital I received:
- A constant drip of the blood thinner heparin
- Had IVs placed in both of my arms
- Had blood drawn at least 40 times (Honestly not sure how I had any blood left.)
- Was put on a central line (A literal IV line in your neck. I would give this experience 0/10 stars, this was honestly the worst part of the entire thing, and I still have a scar on my neck three months later.)
- Underwent a thrombectomy (This is where they stick a tube through an incision they make near your groin, go up to your lungs, and suck out the blood clot). They were able to remove the largest part of the clot, but I’ve had to stay on blood thinners to get rid of the residual clot.
To this day, my doctors aren’t 100 percent sure what the cause was of the pulmonary embolism—and by doctors, I mean the ER doctor, the doctor I had in the hospital, and the hematologist, cardiologist, and pulmonologist I’ve had follow up visits with. Collectively, they all reached the same conclusion: Apri, the birth control pills I had been taking for the last five years up to the day I went into the hospital.
I lost count of how many times I heard in the hospital and during follow-up appointments something along the lines of, “You could have died.” And honestly, I think I’m hearing that so often because the probability of that blood clot killing me was likely much higher than the probability of surviving as I did.
Because of COVID-19, the blood clot grew far larger than it ever should have. Almost two weeks went by from the time I developed symptoms of the clot until the time I was admitted to the ER.
Because of COVID-19, I waited out the week until my test results came back (because of the backlog of tests accumulating in the community it was difficult to get in for a test, and took five days for results to come back) to reach back out to my doctor.
Because of COVID-19, I ignored how bad my symptoms were at home because I didn’t want to go to the hospital unless I really needed to. I didn’t want to take away a bed from someone who really needed it—turns out that person was me.
Because of COVID-19, I spent my ER visit in a hallway and was transferred to an entirely different hospital because there was no space for me.
Because of COVID-19, I had to wait an extra day to have the thrombectomy performed because the surgeon who was initially supposed to perform the procedure went home sick.
I may not have had COVID-19, but I nearly died because of it. Had this happened in November of 2019, my doctor would have told me to go straight to the ER when I first contacted her, and I would have sought help much sooner. Like everyone else, I thought I had COVID.
Three months later, I am just now starting to feel like my normal self again. I still don’t have the same energy I did before, but thankfully, I’m on the road to full recovery.
For the first time in a year, we are starting to see a glimmer of hope in this pandemic as vaccines begin to roll out. But it’s also disheartening to see states like Texas remove mask mandates.
Until enough of the population is vaccinated against COVID-19, we must continue to take measures to protect our communities from COVID-19. Do it in honor of the 500,000+ people who have died from the virus in the United States—let’s please stop adding to that number. Do it for the doctors and nurses who haven’t had a day of rest in the last year. And do it for those suffering from other health emergencies who need the same care they would have gotten before the pandemic.
I’m one of the lucky ones. I lived.
Emily Park is a Kansas City-based journalist, passionate about giving a voice to those who don’t always have one. From news to features to business-to-business reporting, she’s done it all. (Features are her favorite though.) In her free time you can find Emily playing games, reading, streaming, or hanging out with her furry babies, Sutton the dog and Salem the cat.






One thought on “I didn’t have COVID-19, but I almost died because of it”